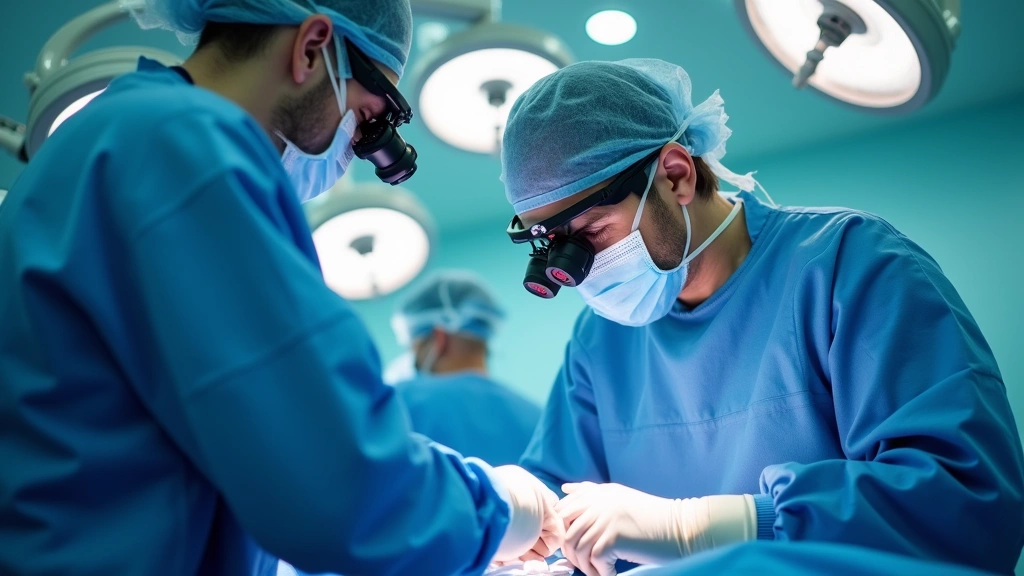
Future of Surgical Tech: Expert Insights Unveiled
The surgical technology landscape is undergoing a revolutionary transformation that promises to redefine how medical professionals approach complex procedures. Advanced surgical tech innovations are reshaping operating rooms worldwide, introducing capabilities that were once confined to science fiction. From robotic-assisted surgery to AI-powered diagnostic systems, the convergence of cutting-edge technology and medical expertise is creating unprecedented opportunities for improved patient outcomes and surgical precision.
Today’s surgeons operate at the intersection of traditional medical knowledge and sophisticated technological advancement. The integration of artificial intelligence, machine learning, and real-time imaging systems represents a fundamental shift in surgical methodology. These advancements not only enhance surgeon capabilities but also reduce procedure duration, minimize tissue trauma, and accelerate patient recovery times. Understanding these developments requires examining the specific technologies driving this evolution and their practical implications for modern healthcare systems.
As we explore the future of surgical technology, we’ll uncover how emerging innovations like artificial intelligence applications are transforming surgical precision and decision-making processes. The expert insights presented here reflect current industry trends, peer-reviewed research, and practical implementations already changing patient care globally.
Robotic-Assisted Surgery Systems
Robotic-assisted surgical systems represent one of the most mature and widely adopted advanced surgical tech innovations in contemporary healthcare. The da Vinci Surgical System, along with emerging competitors like the Hugo RAS and Senhance platform, has fundamentally altered how surgeons execute complex procedures with enhanced dexterity and precision. These systems provide surgeons with magnified three-dimensional visualization, tremor filtering, and intuitive hand controls that translate surgeon movements into precise robotic instrument movements.
The technical specifications of modern surgical robots demonstrate remarkable capabilities. Current generation systems feature multiple articulated arms with up to seven degrees of freedom, far exceeding human wrist flexibility. Force feedback mechanisms allow surgeons to sense tissue resistance, creating a tactile connection that enhances procedural safety. Operating through small incisions reduces patient trauma compared to traditional open surgery, resulting in decreased blood loss, reduced infection risk, and significantly faster recovery periods.
According to The Verge’s technology analysis, robotic surgery adoption has expanded beyond traditional specialties into gynecology, urology, and general surgery. Hospitals implementing these systems report improved surgical outcomes, with some procedures demonstrating 15-30% reduction in complication rates. Training requirements remain substantial, typically requiring 200+ hours of simulation before surgeons perform live procedures, but this investment yields long-term efficiency gains.
The economic model for robotic surgical systems continues evolving. Initial capital investments range from $1.5 to $2.5 million per system, with annual maintenance costs between $100,000 and $150,000. However, increased surgical volume, premium pricing for robotic procedures, and improved operational efficiency create positive return-on-investment scenarios within 3-5 years for high-volume surgical centers.
Artificial Intelligence in the Operating Room
Artificial intelligence integration into surgical workflows represents perhaps the most transformative aspect of future surgical tech development. AI algorithms now assist in pre-operative planning, intra-operative guidance, and post-operative outcome prediction with accuracy rates exceeding 95% in specific applications. Machine learning models trained on thousands of surgical cases can identify optimal procedural approaches, predict complications, and recommend real-time adjustments during surgery.
One particularly promising application involves AI-powered image analysis during procedures. Computer vision systems can identify anatomical structures, detect abnormalities, and highlight critical structures surgeons must preserve. This technology proves especially valuable in cancer surgery, where complete tumor removal while preserving healthy tissue represents the central surgical challenge. AI algorithms analyzing pathology images can identify cancer margins with precision matching or exceeding human pathologists.
Research institutions and major medical device manufacturers are investing heavily in AI surgical applications. CNET’s medical technology coverage highlights how companies like Intuitive Surgical, Stryker, and emerging startups are developing specialized AI modules for specific surgical specialties. Deep learning networks trained on millions of surgical video hours can predict surgeon actions, identify procedural deviations, and flag potential errors before they impact patient safety.
The regulatory pathway for AI surgical systems requires careful validation. FDA approval processes for AI-assisted surgery demand extensive clinical trials demonstrating safety and efficacy improvements over conventional approaches. Current approved systems focus on specific, well-defined tasks rather than autonomous decision-making, reflecting appropriate caution in this critical domain. However, as validation methodologies mature, we expect broader AI integration into surgical workflows.
Advanced Imaging and Visualization
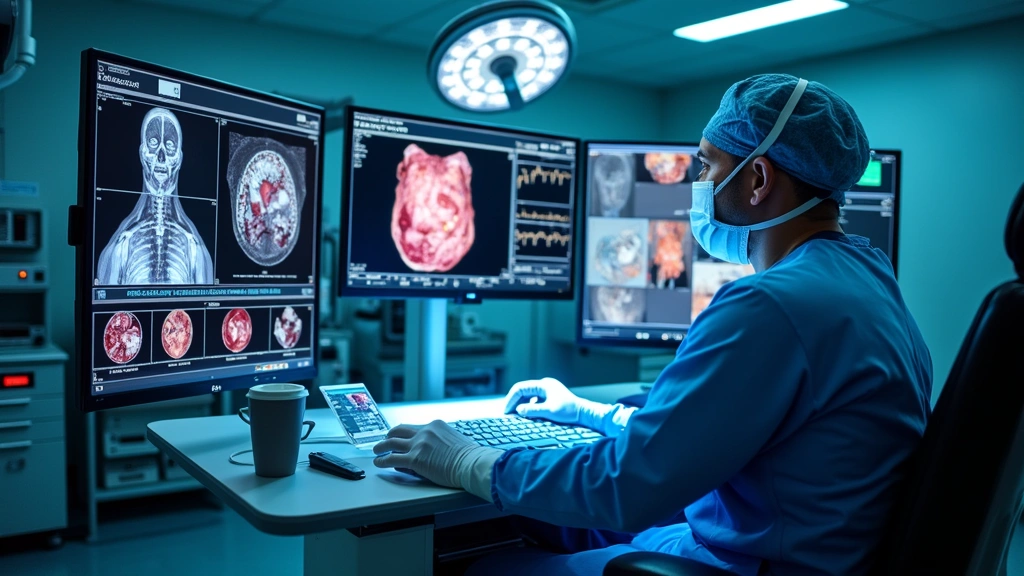
Visualization capabilities represent the foundation of modern surgical technology advancement. High-definition three-dimensional imaging systems, augmented reality overlays, and real-time fluorescence guidance are transforming how surgeons perceive anatomical relationships during procedures. Intraoperative OCT (optical coherence tomography) provides cross-sectional tissue imaging with micrometer resolution, enabling surgeons to visualize structures invisible to naked eye examination.
Augmented reality (AR) surgical systems overlay anatomical data, vascular maps, and tumor boundaries directly onto the surgeon’s field of view. These systems use pre-operative imaging data fused with real-time tracking to maintain accurate anatomical registration throughout procedures. Surgeons can literally see through tissue layers, identifying critical structures and ensuring complete pathology removal while preserving vital anatomy.
Fluorescence-guided surgery represents another significant advancement in surgical visualization. Surgeons inject fluorescent dyes that accumulate in specific tissue types—particularly cancer cells—allowing real-time visualization of tumor margins with remarkable specificity. Near-infrared fluorescence imaging penetrates deeper into tissue than visible light, enabling visualization of sentinel lymph nodes and metastatic disease that conventional imaging might miss.
The technical sophistication of these imaging systems continues accelerating. Integration with artificial intelligence creates intelligent visualization systems that not only display anatomical structures but also provide contextual analysis. These systems can measure tissue dimensions, calculate resection margins, and alert surgeons to anatomical anomalies detected during imaging analysis.
Minimally Invasive Procedures
The minimally invasive surgery revolution continues expanding, driven by advanced surgical tech that enables complex procedures through increasingly smaller incisions. Natural orifice transluminal endoscopic surgery (NOTES), single-port laparoscopy, and micro-invasive approaches are becoming standard for procedures previously requiring large incisions.
These approaches dramatically reduce patient morbidity. Smaller incisions mean less pain, reduced infection risk, faster wound healing, and earlier return to normal activities. Recovery times have compressed from weeks to days in many procedures. Patients experience improved cosmetic outcomes, reduced scarring, and psychological benefits from minimally invasive approaches.
Technical innovations enabling minimally invasive surgery include articulating instruments with multiple degrees of freedom, improved imaging systems providing adequate visualization through tiny ports, and specialized training methodologies. Surgeons must develop new spatial reasoning skills to operate through restricted access points while maintaining procedural accuracy.
The AI applications supporting minimally invasive surgery include real-time guidance systems that help surgeons navigate complex anatomical spaces with limited direct visualization. These systems reduce procedure duration and complication rates, particularly valuable when anatomical complexity increases technical difficulty.
Real-Time Patient Monitoring
Modern surgical tech encompasses sophisticated patient monitoring systems providing real-time physiological data throughout procedures. Advanced anesthesia management systems integrate vital sign monitoring, depth of anesthesia assessment, and predictive analytics identifying potential complications before they develop.
Intraoperative neuromonitoring systems track neural function during procedures affecting nerves, enabling surgeons to preserve nerve function while achieving surgical objectives. These systems use electrical stimulation and recording to continuously assess nerve integrity, alerting surgeons to potential nerve injury risks.
Tissue oximetry monitoring provides real-time assessment of tissue perfusion and oxygenation. This technology proves particularly valuable in reconstructive surgery, where graft survival depends on adequate blood supply. Surgeons can optimize anastomotic techniques and vascular pedicle positioning based on real-time perfusion data.
Integration of these monitoring systems with predictive analytics creates intelligent operating rooms that anticipate complications. Machine learning algorithms analyze real-time physiological data patterns associated with adverse outcomes, alerting surgical teams to emerging problems while interventions remain possible.
Surgical Data Analytics
The transformation of surgical data into actionable insights represents a critical frontier in surgical technology advancement. Hospitals implementing comprehensive surgical data analytics systems achieve measurable improvements in outcomes, efficiency, and safety. These systems capture detailed information about every procedure—duration, resource utilization, complications, outcomes—creating databases enabling continuous improvement.
Predictive analytics applied to surgical data identify risk factors for adverse outcomes specific to individual patients and procedural contexts. Surgeons can adjust operative strategy based on patient-specific risk profiles, potentially preventing complications before they occur. These systems also identify surgeon-specific variation in outcomes, enabling targeted training and technique optimization.
Benchmarking capabilities allow surgical departments to compare their outcomes against regional and national standards. This transparency drives quality improvement initiatives and identifies best practices worthy of adoption. Hospitals can track whether advanced surgical tech implementations actually improve outcomes, ensuring technology investments generate measurable benefits.
The technology innovations in data analytics parallel advancements in other industries, leveraging cloud computing, machine learning, and advanced visualization to transform raw data into strategic insights.
Implementation Challenges
Despite remarkable technological progress, significant barriers to advanced surgical tech adoption persist. Capital costs remain prohibitive for many hospitals, particularly in resource-limited settings. Training requirements demand substantial time investments from surgeons and operating room staff. Regulatory pathways for novel surgical technologies can be lengthy and uncertain, delaying beneficial innovations from reaching patients.
Cybersecurity represents an emerging critical concern. Connected surgical systems create potential vulnerabilities that malicious actors might exploit. Ransomware attacks targeting hospital networks could compromise surgical robot functionality or patient data. Manufacturers and healthcare institutions must implement robust security protocols protecting these critical systems.
Surgeon acceptance varies considerably. Some practitioners embrace technological advancement enthusiastically, while others express concern about technology dependence or concern that advanced systems might reduce surgical skill development. Optimal outcomes require thoughtful integration of technology with traditional surgical expertise rather than wholesale replacement of human judgment.
Regulatory frameworks struggle to keep pace with rapid technological innovation. Current FDA approval processes, designed for incremental improvements to established device categories, may be ill-suited for truly novel surgical technologies. Balancing innovation acceleration with appropriate safety oversight remains an ongoing challenge.
Healthcare systems must also address equity considerations. Advanced surgical tech adoption may increase disparities in care access if primarily available at well-funded academic centers. Ensuring equitable access to technological benefits across diverse healthcare settings remains an important societal challenge.
Future Outlook and Emerging Technologies
The trajectory of surgical technology development suggests even more remarkable innovations approaching clinical implementation. Fully autonomous surgical robots capable of performing specific procedures without real-time surgeon control represent active research areas. These systems would combine advanced imaging, AI decision-making, and robotic precision to execute optimal surgical technique consistently.
Extended reality (XR) technologies—combining virtual reality, augmented reality, and mixed reality—promise immersive surgical training and intraoperative guidance. Surgeons could practice complex procedures virtually before performing them on actual patients, dramatically reducing learning curves and improving initial outcomes.
Tissue engineering integration with surgical technology may enable intraoperative fabrication of tissue scaffolds or regenerative materials. Surgeons could potentially print patient-specific tissue replacements during procedures, revolutionizing reconstructive and transplant surgery.
Nanotechnology applications in surgery remain largely theoretical but offer tantalizing possibilities. Nanorobots could theoretically perform surgery at cellular levels, though significant technological and regulatory barriers must be overcome before clinical implementation.
The convergence of technology innovations with surgical practice will continue accelerating. However, human expertise, clinical judgment, and ethical considerations must remain central to surgical technology development. The most successful surgical tech implementations will be those thoughtfully integrating technological capabilities with the irreplaceable value of experienced surgical expertise.

FAQ
What is robotic-assisted surgery and how does it differ from traditional surgery?
Robotic-assisted surgery utilizes specialized robotic systems controlled by surgeons to perform procedures through small incisions. Unlike traditional open surgery requiring large incisions, robotic systems enable minimally invasive approaches with enhanced visualization, tremor filtering, and precise instrument control. Surgeons maintain complete control throughout procedures while benefiting from improved dexterity and visualization capabilities.
How is artificial intelligence used in surgical procedures?
AI assists surgeons through multiple mechanisms: pre-operative planning optimization, intraoperative image analysis identifying critical structures and tumor margins, real-time guidance systems, and predictive analytics flagging potential complications. AI algorithms trained on thousands of surgical cases can recognize patterns and recommend approaches based on patient-specific factors, enhancing surgical decision-making.
What are the main benefits of advanced surgical technology?
Key benefits include improved surgical precision reducing complication rates, minimally invasive approaches enabling faster recovery, real-time monitoring enhancing patient safety, and data analytics driving continuous quality improvement. Patients experience reduced pain, shorter hospital stays, faster return to normal activities, and improved cosmetic outcomes compared to traditional surgical approaches.
How much do robotic surgical systems cost?
Initial capital investment for robotic surgical systems ranges from $1.5 to $2.5 million per unit. Annual maintenance costs typically range from $100,000 to $150,000. Despite substantial upfront costs, high-volume surgical centers achieve positive return-on-investment within 3-5 years through increased surgical volume and premium pricing for robotic procedures.
What training is required for surgeons using advanced surgical technology?
Surgeon training requirements vary by technology but typically involve 200+ hours of simulation before performing live procedures. Training encompasses understanding system mechanics, developing spatial reasoning skills for minimally invasive approaches, and integrating technology capabilities with traditional surgical expertise. Ongoing education keeps surgeons current with evolving technological capabilities.
Are there safety concerns with AI-assisted surgery?
Safety represents paramount concern in surgical AI development. Current approved systems focus on specific, well-defined tasks rather than autonomous decision-making. Extensive validation through clinical trials demonstrates safety improvements before regulatory approval. Cybersecurity protocols protect systems from potential vulnerabilities. Surgeon oversight remains essential, with AI functioning as a decision-support tool rather than autonomous agent.
Will advanced surgical technology replace human surgeons?
No. Advanced surgical technology augments surgeon capabilities rather than replacing human expertise. Surgical judgment, ethical decision-making, adaptability to unexpected circumstances, and patient communication require human surgeons. The most successful implementations combine technological precision with experienced surgical expertise, creating synergistic improvements in patient outcomes.
How do minimally invasive surgical techniques improve patient recovery?
Smaller incisions reduce tissue trauma, blood loss, and infection risk. Patients experience less postoperative pain, faster wound healing, and earlier mobilization. Hospital stays compress from weeks to days, and return to normal activities accelerates from months to weeks. Improved cosmetic outcomes and psychological benefits from less invasive approaches enhance overall patient satisfaction.
What future surgical technologies are in development?
Emerging technologies include fully autonomous surgical robots, extended reality training and guidance systems, intraoperative tissue fabrication, and nanotechnology applications. These innovations promise further improvements in surgical precision, training effectiveness, and patient outcomes. However, significant technological and regulatory barriers must be overcome before widespread clinical implementation.
How does surgical data analytics improve patient outcomes?
Surgical data analytics capture detailed information about procedures, enabling identification of risk factors, outcome prediction, and best practice recognition. Surgeons can adjust strategy based on patient-specific risk profiles. Benchmarking against standards drives quality improvement initiatives. Continuous analysis identifies opportunities for technique optimization and complication prevention, systematically improving surgical program performance.