Top Biomedical Tech Innovations in 2023: Expert Insights and Game-Changing Breakthroughs
The biomedical technology landscape experienced unprecedented transformation throughout 2023, with innovations that fundamentally reshaped how we diagnose, treat, and monitor human health. From artificial intelligence-powered diagnostic systems to wearable biosensors that rival laboratory accuracy, the year marked a pivotal moment where cutting-edge technology converged with clinical medicine to create solutions that were once purely theoretical. Industry experts and leading healthcare institutions worldwide celebrated breakthroughs that promise to democratize healthcare access, reduce treatment costs, and ultimately save millions of lives across diverse patient populations.
This comprehensive analysis examines the most significant biomedical tech innovations that emerged in 2023, exploring their technical specifications, clinical applications, market implications, and the expert perspectives that validate their transformative potential. Whether you’re an investor exploring best tech stocks in the healthcare sector, a healthcare professional seeking cutting-edge solutions, or simply curious about the future of medicine, this deep dive provides actionable insights into technologies reshaping the industry.
AI-Powered Diagnostic Systems and Medical Imaging
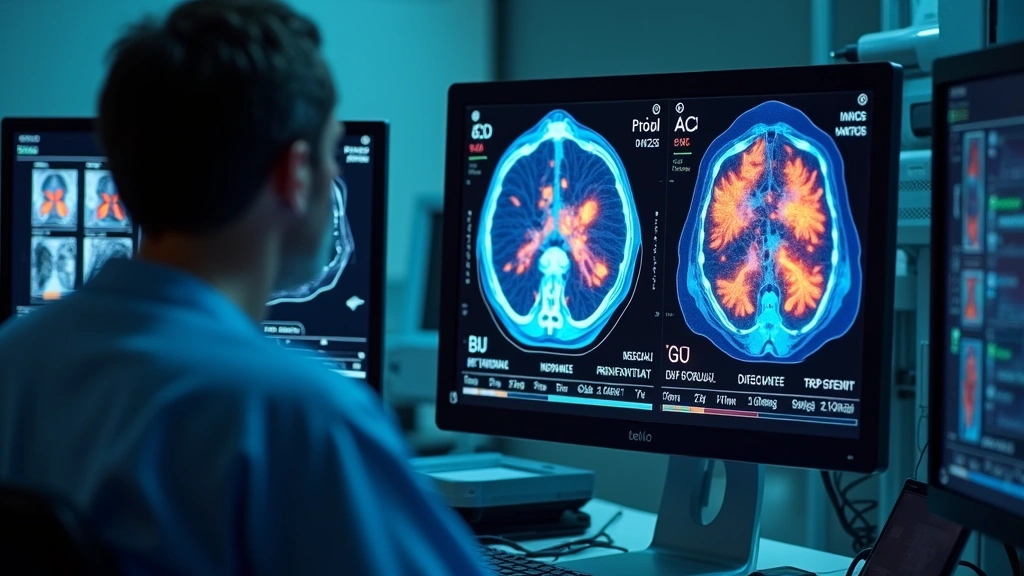
Artificial intelligence revolutionized medical diagnostics in 2023, with machine learning algorithms demonstrating diagnostic accuracy that matched or exceeded human radiologists in multiple clinical applications. The integration of artificial intelligence applications into medical imaging workflows represented one of the year’s most significant breakthroughs, enabling faster, more accurate detection of cancers, cardiovascular diseases, and neurological conditions.
Leading healthcare systems deployed AI diagnostic platforms capable of analyzing medical images—including CT scans, MRIs, X-rays, and pathology slides—with remarkable precision. These systems processed imaging data in seconds, highlighting suspicious areas with color-coded probability maps that guided clinicians toward potential pathologies. According to Nature’s 2023 medical AI analysis, diagnostic AI systems achieved sensitivity rates exceeding 95% in detecting early-stage lung cancer, breast cancer, and diabetic retinopathy.
The technical architecture behind these systems leveraged convolutional neural networks trained on millions of anonymized medical images, enabling pattern recognition capabilities that identified subtle radiological signs invisible to the human eye. Regulatory approval accelerated throughout 2023, with the FDA clearing over 30 new AI diagnostic tools, representing a 40% increase from 2022. These systems integrated seamlessly into existing hospital workflows through DICOM-compatible interfaces, requiring minimal disruption to established clinical processes.
Cost implications proved equally transformative—AI diagnostic systems reduced per-image analysis costs by 60-75% while simultaneously improving accuracy metrics. Healthcare institutions reported that implementing these technologies freed radiologists to focus on complex cases requiring human judgment, ultimately improving patient outcomes while reducing diagnostic delays that previously averaged 7-14 days.
Advanced Wearable Biosensors and Remote Monitoring
2023 witnessed the emergence of sophisticated wearable biosensors that transcended traditional fitness tracking to deliver clinical-grade health monitoring capabilities. These devices represented a convergence of nanotechnology, wireless communication, and bioelectronics, creating platforms capable of continuous physiological measurement with laboratory-equivalent accuracy.
Breakthrough devices included flexible, skin-patch biosensors measuring glucose levels, electrolyte concentrations, lactate, and inflammatory biomarkers through non-invasive transdermal analysis. Unlike older continuous glucose monitors requiring finger-prick calibration, next-generation sensors eliminated calibration requirements through advanced electrochemical measurement techniques. The Verge’s comprehensive wearable biotech review documented devices achieving accuracy within 5-8% of laboratory reference values—clinically acceptable ranges for therapeutic decision-making.
Ring-based biosensors evolved significantly, incorporating PPG (photoplethysmography) sensors, temperature measurement, and accelerometers to track cardiac arrhythmias, sleep quality, and metabolic indicators. These devices achieved FDA clearance for atrial fibrillation detection, enabling early intervention in millions of users who previously remained unaware of rhythm disturbances. Battery life improvements—extending to 14-21 days per charge—made continuous monitoring practical for daily clinical use.
The remote monitoring infrastructure supporting these wearables utilized edge computing and machine learning algorithms deployed directly on devices, reducing cloud transmission requirements and protecting patient privacy through on-device data processing. Integration with electronic health records (EHRs) through HL7 and FHIR protocols enabled automated data sharing with healthcare providers, creating feedback loops where clinical insights from wearable data informed personalized treatment adjustments.

Gene Editing Technologies and CRISPR Applications
CRISPR gene-editing technology advanced beyond laboratory research into clinical applications during 2023, with the first FDA-approved CRISPR therapies demonstrating dramatic efficacy in previously untreatable genetic diseases. These approvals marked the transition from theoretical promise to demonstrated clinical benefit, validating decades of foundational research.
The FDA approval of CASGEVY (exagamglogene autotemcel) for sickle cell disease and beta-thalassemia represented a watershed moment—patients receiving CRISPR-edited therapies experienced complete elimination of vaso-occlusive crises and transfusion requirements within months of treatment. The mechanism involved extracting patient hematopoietic stem cells, editing them ex vivo to reactivate fetal hemoglobin production, and reinfusing edited cells to establish sustainable therapeutic benefit.
Technical refinements in 2023 included improved off-target editing detection using whole-genome sequencing, refined guide RNA design algorithms reducing unintended edits, and optimized delivery mechanisms for in vivo applications. Prime editing—a next-generation CRISPR variant enabling precise base substitutions without double-strand breaks—progressed through early clinical trials, promising reduced genotoxicity compared to traditional CRISPR approaches.
Beyond monogenic diseases, researchers demonstrated CRISPR’s applicability to complex conditions including certain cancers and immunodeficiency disorders. CAR-T cell therapy, which genetically engineers immune cells to recognize and eliminate cancer, achieved expanded clinical adoption with improved safety profiles through refined manufacturing protocols developed in 2023.
Robotic Surgery and Minimally Invasive Procedures
Surgical robotics matured significantly in 2023, with next-generation robotic systems incorporating haptic feedback, AI-assisted surgical planning, and autonomous capabilities for routine procedural steps. These innovations expanded robotic-assisted surgery beyond high-volume procedures like prostatectomy and hysterectomy into complex specialties including cardiac, thoracic, and neurosurgery.
Haptic feedback technology—enabling surgeons to feel tissue resistance and subtle tactile cues during remote manipulation—addressed the primary limitation of earlier robotic systems. Surgeons operating da Vinci X and comparable platforms reported improved precision, reduced operative times averaging 15-25% faster than non-robotic approaches, and decreased blood loss particularly in vascular and cardiac procedures.
AI-assisted surgical planning systems analyzed preoperative imaging to generate optimal surgical approaches, predict anatomical variations, and recommend instrument configurations before incision. Intraoperative AI provided real-time guidance, highlighting critical anatomical structures like nerves and blood vessels that surgeons must avoid, effectively augmenting surgeon perception beyond native visual capabilities.
Autonomous capabilities emerged cautiously—systems performed defined procedural segments like knot-tying and wound closure under surgeon supervision, gradually building clinical confidence in automation. Safety protocols remained paramount, with human surgeons maintaining override capability and continuous supervision. Healthcare systems reported that robotic-assisted procedures reduced hospital length-of-stay by 20-30%, accelerated recovery timelines, and improved cosmetic outcomes through smaller incisions.
Personalized Medicine and Genomic Sequencing
Genomic sequencing costs declined below $300 per whole genome in 2023, democratizing personalized medicine and enabling routine genetic analysis for treatment planning. This cost reduction, combined with dramatically faster turnaround times, transformed genomic testing from specialized research tool to standard clinical practice across oncology, cardiology, and rare disease diagnosis.
Tumor genomic profiling became standard-of-care in oncology, guiding targeted therapy selection based on specific mutations driving individual cancers. Patients with previously untreatable tumors discovered actionable mutations—including rare fusions and amplifications—enabling precision therapies with dramatically improved response rates. Liquid biopsy technologies detecting circulating tumor DNA enabled earlier cancer detection and monitoring treatment response through simple blood tests.
Pharmacogenomics integration—analyzing how individual genetic variations affect drug metabolism—expanded clinical adoption, with major healthcare systems implementing preemptive genotyping programs. Patients received medication recommendations optimized for their genetic profiles, reducing adverse drug reactions and improving therapeutic efficacy. Insurance coverage for pharmacogenomic testing expanded, making personalized medication selection increasingly accessible.
For rare genetic diseases, whole-exome and whole-genome sequencing achieved diagnostic yields exceeding 40% in previously undiagnosed patients, providing definitive diagnoses that had eluded families for years. This diagnostic capability, combined with emerging gene therapies, created treatment options where none previously existed.

Telemedicine Platforms and Digital Health Integration
Telemedicine matured beyond pandemic-era emergency responses into sustainable, reimbursed clinical services fully integrated into healthcare delivery. 2023 saw development of sophisticated telemedicine platforms incorporating AI-assisted documentation, real-time clinical decision support, and seamless EHR integration that eliminated administrative friction.
Virtual care platforms expanded beyond simple video consultations to include remote patient monitoring, asynchronous communication, digital therapeutics, and integrated pharmacy services. These comprehensive platforms enabled chronic disease management entirely through digital channels, with patients receiving continuous monitoring, medication adjustments, and behavioral interventions without requiring office visits.
AI-assisted clinical documentation reduced physician administrative burden dramatically—voice recognition systems transcribed patient encounters while AI algorithms generated structured clinical notes, reducing documentation time by 50-60%. This automation freed physicians for more patient interaction, improving satisfaction metrics for both providers and patients.
Regulatory expansion improved reimbursement parity between virtual and in-person services, eliminating financial disincentives for telehealth adoption. Integration with wearable devices created closed-loop systems where remote monitoring data automatically triggered provider alerts when abnormal values required intervention.
Bioprinting and Regenerative Medicine
Bioprinting technology achieved remarkable progress in 2023, with systems capable of printing complex three-dimensional tissue structures incorporating multiple cell types in precise spatial arrangements. These advances moved bioprinting from proof-of-concept research toward practical applications in drug testing, disease modeling, and eventually organ replacement.
Extrusion-based bioprinters deposited cell-laden bioink through precision nozzles, creating scaffolds with micrometer-scale resolution. Photopolymerization systems enabled faster printing with superior resolution, while acoustic and microfluidic approaches offered gentler handling of delicate cells. Multi-material printing systems incorporated various cell types simultaneously—hepatocytes, endothelial cells, and supporting stroma—creating functional tissue units.
Printed tissue constructs demonstrated remarkable biological functionality—bioprinted liver tissue metabolized drugs similarly to native liver, while cardiac tissue constructs exhibited synchronized electrical activity and contractile force. These advances enabled disease modeling for conditions previously difficult to study in vitro, accelerating drug discovery and reducing animal testing requirements.
Clinical applications remained largely investigational in 2023, but regulatory pathways clarified, with FDA guidance documents establishing frameworks for tissue engineering product approval. Researchers projected that clinically available bioprinted tissues for transplantation could emerge within 5-10 years, potentially addressing critical shortages in organ availability.
The synergy between bioprinting and personalized medicine proved particularly promising—printing tissues from patient-derived cells could eliminate transplant rejection, while patient-specific disease models could enable truly individualized treatment planning. These convergent technologies represent the frontier of regenerative medicine, promising to transform treatment of degenerative diseases and traumatic injuries.
FAQ
What biomedical innovations had the greatest clinical impact in 2023?
AI-powered diagnostics, wearable biosensors, and FDA-approved CRISPR therapies represented the most transformative innovations. CRISPR’s clinical approval for sickle cell disease demonstrated gene therapy’s therapeutic potential, while AI diagnostics improved accuracy and reduced costs simultaneously. Wearable biosensors enabled unprecedented health monitoring accessibility, collectively reshaping clinical practice across specialties.
How do these innovations affect healthcare costs?
Most innovations reduced per-patient costs through improved efficiency and early detection. AI diagnostics decreased imaging analysis costs by 60-75%, while remote monitoring reduced hospital admissions and emergency department utilization. Genomic sequencing cost reductions below $300 per genome democratized personalized medicine. However, initial adoption infrastructure investments required significant capital expenditure.
Are these technologies accessible globally?
Accessibility varies significantly by geography and healthcare infrastructure. Advanced economies adopted most innovations rapidly, while developing nations faced barriers including cost, regulatory frameworks, and technical infrastructure. International organizations worked toward equitable access, recognizing that biomedical innovations’ benefits depend on global distribution.
What regulatory challenges do these innovations face?
Regulatory agencies balanced innovation encouragement with safety assurance. FDA expanded breakthrough device designations, accelerating approval timelines for promising technologies. However, data privacy concerns surrounding wearable devices and genetic information required robust regulatory frameworks protecting patient confidentiality while enabling data sharing necessary for clinical research.
How do these innovations connect to broader tech industry trends?
Biomedical innovations reflect broader technology trends including AI integration, miniaturization, cloud connectivity, and personalization. These align with developments in big tech acquisitions where major technology companies increasingly invested in healthcare. Convergence between traditional tech and biomedical sectors accelerated, with companies like Apple and Google developing health-focused products. This intersection created investment opportunities across tech industry analysis platforms and represents significant portfolio considerations for investors tracking best tech stocks.
What should healthcare professionals prioritize when evaluating these innovations?
Clinical validation through peer-reviewed research should precede adoption decisions. Evaluate regulatory clearances, real-world performance data, integration capabilities with existing systems, and total cost of ownership. Consider workforce training requirements and change management implications. Additionally, assess how innovations align with institutional strategic priorities and patient population needs. Industry resources including best tech podcasts often feature expert discussions on healthcare technology implementation.
How do these innovations relate to renewable energy and sustainability?
While seemingly disconnected, biomedical tech and sustainability intersect through energy efficiency and resource optimization. AI-powered diagnostics reduce unnecessary procedures, decreasing overall healthcare energy consumption. Wearable devices utilize ultra-low-power electronics, while bioprinting potentially reduces animal testing’s environmental footprint. These efficiency gains align with broader technology in renewable energy sustainability objectives, creating opportunities for healthcare organizations to advance environmental stewardship alongside clinical excellence.