Top Cath Lab Gadgets: Expert Insights on Cardiac Catheterization Technology
Cardiac catheterization laboratories have evolved dramatically over the past decade, transforming from basic diagnostic spaces into sophisticated intervention suites equipped with cutting-edge medical technology. The modern cath lab represents a convergence of advanced imaging systems, real-time monitoring devices, and precision instruments that enable cardiologists to diagnose and treat complex heart conditions with unprecedented accuracy. Whether you’re a healthcare administrator evaluating equipment investments, a clinical engineer managing cath lab operations, or a cardiology professional staying current with technological advances, understanding the latest cath lab tech innovations is essential for optimizing patient outcomes and operational efficiency.
The integration of artificial intelligence, advanced imaging modalities, and wireless monitoring systems has revolutionized how interventional cardiologists approach patient care. Modern cath lab gadgets now provide real-time hemodynamic data, three-dimensional anatomical visualization, and automated decision-support systems that enhance procedural safety and effectiveness. This comprehensive guide explores the most significant technological innovations currently transforming cardiac catheterization laboratories worldwide, offering expert perspectives on implementation, clinical benefits, and future trends shaping interventional cardiology.
Advanced Imaging Systems and Visualization Technology
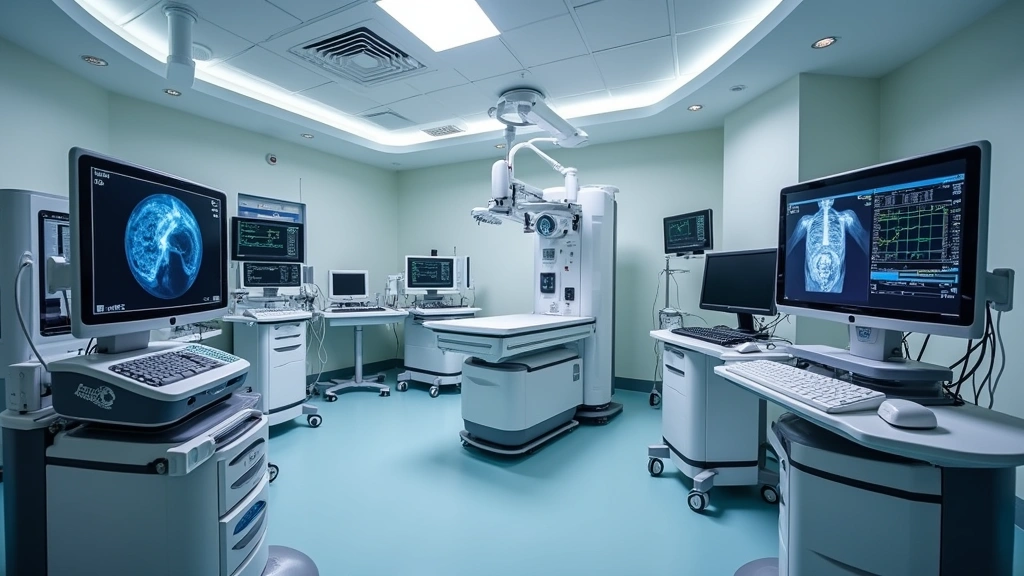
The cornerstone of modern cath lab technology centers on advanced imaging systems that provide unprecedented visualization of coronary anatomy and cardiac structures. Contemporary interventional cardiology relies heavily on multimodal imaging, combining fluoroscopy, intravascular ultrasound (IVUS), optical coherence tomography (OCT), and rotational angiography to create comprehensive three-dimensional maps of the coronary tree.
High-definition flat-panel detectors have become standard in modern cath labs, offering superior image quality with reduced radiation exposure compared to older image intensifier technology. These systems capture images at 30 frames per second with enhanced spatial resolution, enabling clinicians to identify subtle anatomical features, calcification patterns, and optimal intervention angles with remarkable precision. The integration of artificial intelligence applications transforming diagnostic imaging has introduced automated vessel detection algorithms that highlight coronary lesions and suggest optimal viewing angles, significantly reducing procedure times and radiation doses.
Optical coherence tomography represents a transformative imaging modality offering near-histologic resolution of coronary plaque composition. OCT systems can differentiate between lipid-rich plaques, fibrous tissue, and calcification, providing critical information for stent sizing and positioning. Modern OCT pullback systems operate at speeds up to 20mm per second, capturing detailed cross-sectional images of extended coronary segments. CNET’s health technology coverage highlights innovations in medical imaging, noting how OCT integration has reduced stent restenosis rates by improving deployment precision.
Intravascular ultrasound continues to play a vital role in complex interventions, providing real-time cross-sectional imaging that guides stent sizing, identifies calcium burden, and detects hazardous plaque morphologies. Advanced IVUS systems now feature integrated software that automatically measures lumen and stent dimensions, reducing manual measurement variability and improving consistency across different operators.

Hemodynamic Monitoring and Real-Time Data Analytics
Sophisticated hemodynamic monitoring systems form the nervous system of the modern cath lab, continuously tracking pressure gradients, oxygen saturation, cardiac output, and perfusion parameters throughout interventional procedures. Contemporary hemodynamic platforms integrate data from multiple sensors, providing clinicians with comprehensive physiological profiles that inform real-time decision-making.
Fractional flow reserve (FFR) technology has revolutionized coronary lesion assessment by enabling pressure-wire guided intervention. Modern FFR systems provide instantaneous measurements of coronary pressure gradients, allowing interventionalists to determine whether borderline lesions require intervention or can be safely managed medically. Instantaneous wave-free ratio (iFR) represents an alternative pressure measurement technique that eliminates the need for adenosine administration, reducing procedure time and improving patient comfort. These advanced diagnostic tools from leading medical device manufacturers now feature wireless data transmission and cloud-based analysis platforms that enable remote consultation and decision support.
Real-time hemodynamic analytics platforms synthesize data from pressure sensors, flow meters, oxygen saturation monitors, and cardiac output devices into integrated dashboards that display comprehensive physiological trends. Machine learning algorithms analyze this data stream to identify hemodynamic deterioration patterns, automatically alerting the clinical team to potential complications before they become clinically apparent. This predictive capability has proven particularly valuable in managing high-risk patients and complex procedures where hemodynamic stability is precarious.
Advanced cardiac output monitoring using thermodilution or non-invasive techniques enables continuous assessment of systemic perfusion during procedures. Integration of these measurements with real-time arterial pressure monitoring and peripheral perfusion metrics provides comprehensive hemodynamic characterization that guides fluid management and inotropic support decisions.
Interventional Devices and Guidewire Technology
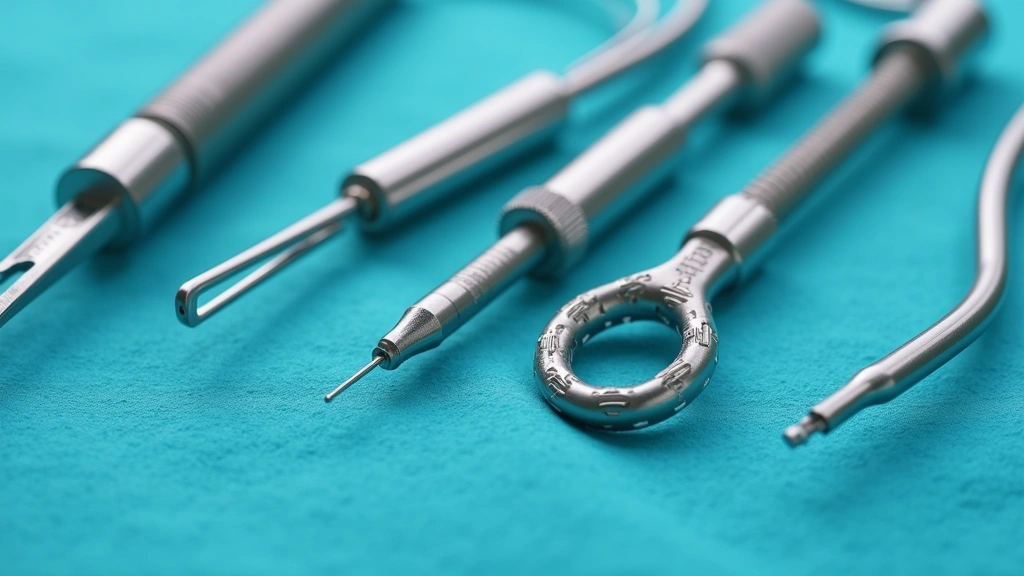
The evolution of interventional devices represents perhaps the most visible advancement in contemporary cath lab technology and medical innovation. Modern guidewires feature sophisticated core designs combining radiopacity, trackability, and support characteristics optimized for specific anatomical challenges. Polymer-jacketed wires with hydrophilic coatings enable passage through tortuous vessels and calcified lesions that would have been impossible to cross with earlier generation devices.
Drug-eluting stent technology has matured dramatically, with contemporary iterations featuring bioabsorbable polymers, thin-strut designs, and specialized surface modifications that reduce thrombosis risk while promoting endothelial healing. Bioresorbable vascular scaffolds represent an emerging frontier, providing temporary structural support that gradually resorbs, potentially restoring normal vessel physiology. Leading cardiovascular device manufacturers continue advancing stent technology through material science innovations and computational design optimization.
Rotational atherectomy systems enable intervention in heavily calcified lesions that resist conventional balloon angioplasty. Modern rotational atherectomy devices feature advanced burr designs, improved rotational stability, and real-time ablation monitoring that enables safer, more efficient calcium removal. Orbital atherectomy represents an alternative approach utilizing eccentric orbital motion to selectively ablate calcification while preserving healthy vessel wall.
Aspiration thrombectomy devices continue evolving to improve thrombus removal in acute coronary syndromes. Contemporary systems feature larger bore catheters, improved aspiration force control, and integrated imaging capabilities that enable real-time assessment of thrombus burden and removal efficacy.
Radiation Safety and Dose Management Systems
Radiation protection has become increasingly sophisticated in modern cath labs, with comprehensive dose management systems tracking cumulative patient exposure and optimizing imaging protocols to minimize radiation burden. Real-time dose monitoring displays integrated into angiography systems provide immediate feedback on radiation output, enabling operators to reduce fluoroscopy time and frame rates when clinically appropriate.
Pulsed fluoroscopy reduces radiation dose by 50-75% compared to continuous fluoroscopy, and modern systems intelligently alternate between pulsed and continuous modes based on procedural requirements. Frame rate optimization algorithms automatically adjust image acquisition frequency based on motion dynamics, capturing rapid motion at higher frame rates while reducing frame rate during stable periods.
Automated collimation systems minimize unnecessary radiation field size, reducing scattered radiation exposure to patient organs and operator hands. Lead-free apron technology provides equivalent radiation protection to traditional lead while reducing weight and improving ergonomics for interventional cardiologists who wear protective equipment during hundreds of procedures annually.
Dose tracking software maintains detailed records of cumulative radiation exposure across all cath lab procedures, enabling institution-wide analysis of radiation practices and identification of opportunities for dose reduction. This data informs staff training, equipment upgrades, and protocol modifications aimed at optimizing the balance between diagnostic image quality and radiation safety.
Robotic-Assisted Catheterization Systems
Robotic assistance in cath lab procedures represents a paradigm shift in interventional cardiology, offering potential advantages in catheter control, reproducibility, and operator ergonomics. Remote catheter navigation systems enable operators to control guidewire and catheter movement with enhanced precision, reducing manual manipulation and associated complications. Medtronic and other device manufacturers are advancing robotic interventional platforms that integrate haptic feedback, allowing operators to sense tissue resistance and procedural forces despite remote control positioning.
Robotic systems demonstrate particular utility in complex anatomies including severely tortuous vessels, challenging left main stenoses, and saphenous vein graft interventions. The precision of robotic catheter advancement reduces procedure time and radiation exposure compared to manual techniques, particularly in cases requiring extensive guidewire manipulation.
Telerobotics enables interventional cardiologists to perform procedures from remote locations, potentially expanding access to specialized interventional expertise in underserved regions. Early telerobotics experiences have demonstrated technical feasibility, though regulatory frameworks and reimbursement models continue evolving to support widespread adoption.
Artificial Intelligence Integration in Cath Labs
The integration of artificial intelligence transforming healthcare delivery and clinical decision-making has introduced powerful diagnostic and analytical capabilities to cath lab operations. Machine learning algorithms trained on thousands of angiographic studies can automatically detect coronary lesions, quantify stenosis severity, and identify anatomical variations that might be subtle on visual inspection alone.
AI-powered vessel tracking algorithms automatically identify and follow coronary arteries throughout angiographic sequences, enabling automated quantitative coronary angiography without manual operator intervention. These systems measure lesion length, reference diameter, and percentage stenosis with consistency exceeding manual measurements, reducing inter-observer variability and improving lesion characterization reproducibility.
Predictive analytics platforms analyze patient demographics, procedural characteristics, and real-time hemodynamic data to identify high-risk patients and estimate procedural complication probability. These predictions enable proactive risk mitigation strategies and inform informed consent discussions with patients regarding procedure-specific risks.
Natural language processing systems automatically extract relevant clinical information from procedural reports, enabling structured data capture that facilitates outcome tracking, quality improvement initiatives, and clinical research without imposing additional documentation burden on clinicians.
Wireless Monitoring and Data Integration Platforms
Modern cath labs increasingly feature wireless monitoring systems that eliminate bedside monitoring cable clutter while enabling seamless data integration across institutional networks. Wireless hemodynamic monitors transmit real-time pressure, oxygen saturation, and cardiac output data directly to the angiography system and electronic health record, enabling comprehensive data capture without manual transcription.
Cloud-based cath lab data platforms aggregate procedural information, imaging data, hemodynamic parameters, and outcomes across multiple institutions, enabling benchmarking against peer institutions and identification of best practices. These platforms support collaborative learning through anonymous case sharing, enabling clinicians to learn from colleagues’ experiences and procedural approaches.
Integration of data management and analysis capabilities with cath lab systems enables automated outcome tracking and quality improvement feedback loops. Real-time dashboards display institution-specific metrics including procedure success rates, complication frequencies, radiation doses, and contrast utilization, enabling continuous performance monitoring and rapid identification of improvement opportunities.
Implementation Considerations and ROI Analysis
Healthcare administrators evaluating cath lab technology investments must carefully balance clinical benefits against significant capital expenditures and ongoing operational costs. Advanced imaging systems, hemodynamic monitors, and robotic platforms represent substantial investments requiring careful justification through clinical outcome improvements and operational efficiency gains.
Return on investment analysis should encompass multiple dimensions including reduced procedure times (decreasing staff costs and increasing daily case volume), improved clinical outcomes (reducing complications and associated treatment costs), enhanced radiation safety (reducing occupational exposure), and improved staff ergonomics (reducing occupational injuries and burnout). Institutions implementing comprehensive technology upgrades often realize procedure time reductions of 15-25%, translating to meaningful volume increases and cost reductions.
Training requirements for advanced cath lab technologies warrant careful planning and resource allocation. Interventional cardiologists and clinical staff require structured education programs to achieve proficiency with new imaging modalities, hemodynamic monitoring platforms, and artificial intelligence-assisted decision support systems. Manufacturer training programs, peer mentoring from experienced operators, and simulation-based learning have all proven effective for technology adoption.
Regulatory compliance considerations including FDA approvals, institutional credentialing requirements, and quality assurance protocols must be addressed prior to implementing new cath lab technologies. Institutions should establish clear governance structures for technology evaluation, procurement, and clinical integration to ensure systematic assessment and appropriate utilization.
The future of technology investments in healthcare and medical innovation increasingly emphasizes interoperability and data integration rather than isolated point-of-care devices. Cath labs adopting comprehensive digital ecosystems that integrate imaging, hemodynamics, electronic health records, and quality tracking platforms realize greater value than those implementing technology in fragmented approaches.
Sustainability considerations including device lifecycle management, recycling programs, and energy efficiency should inform technology selection decisions. Modern cath lab systems increasingly feature power management capabilities that reduce energy consumption during periods of reduced utilization, aligning operational efficiency with environmental stewardship.
Integration of advanced technology innovations and sustainable practices in healthcare settings reflects broader institutional commitments to environmental responsibility while maintaining clinical excellence. Cath labs incorporating energy-efficient imaging systems, wireless technologies reducing material waste, and digital documentation systems demonstrate commitment to sustainable healthcare delivery.
FAQ
What is the most critical advancement in modern cath lab technology?
Advanced imaging systems, particularly high-definition flat-panel detectors and optical coherence tomography, represent the most transformative advancement, enabling unprecedented visualization of coronary anatomy and plaque composition. These technologies directly improve interventional outcomes through enhanced lesion characterization and optimal device positioning.
How do hemodynamic monitoring systems improve patient outcomes?
Real-time hemodynamic monitoring enables early detection of physiological deterioration, guides fluid and inotropic management decisions, and provides objective data for lesion assessment through fractional flow reserve measurements. These capabilities reduce complications and improve procedural decision-making in complex cases.
Are robotic-assisted cath lab systems ready for widespread adoption?
Robotic systems demonstrate clear advantages in specific complex anatomies and show promise for reducing procedure time and radiation exposure. However, widespread adoption requires further evidence of cost-effectiveness, expanded clinical applications, and resolution of regulatory and reimbursement frameworks.
What training is required for operators to effectively utilize advanced cath lab technologies?
Comprehensive training programs encompassing didactic education, hands-on system demonstrations, simulation-based learning, and supervised clinical cases enable operators to achieve proficiency with advanced technologies. Ongoing education programs ensure continued competency as technologies evolve.
How can institutions ensure successful technology implementation in cath labs?
Successful implementation requires clear governance structures, comprehensive needs assessment, vendor selection based on institutional priorities, structured training programs, quality assurance protocols, and ongoing performance monitoring. Engaging clinical staff early in technology evaluation and implementation planning improves adoption rates and utilization.
What future developments will most significantly impact cath lab practice?
Integration of artificial intelligence for automated image analysis, expansion of robotic-assisted interventions, development of bioresorbable scaffolds, and implementation of comprehensive digital ecosystems connecting cath labs with broader institutional systems will shape future practice. These advances will collectively enhance safety, efficiency, and clinical outcomes.