Is Anesthesia Tech Safe? Expert Insights on Medical Device Safety
Anesthesia technology has revolutionized surgical procedures over the past century, enabling complex operations that would otherwise be impossible. Modern anesthesia delivery systems combine precision hardware, sophisticated software, and real-time monitoring capabilities to keep patients safe during procedures. However, as with all medical technologies, questions about safety, reliability, and potential risks remain paramount. This comprehensive guide examines the current state of anesthesia technology, regulatory frameworks, and expert perspectives on whether these critical systems meet the highest safety standards.
The evolution of anesthesia tech represents one of medicine’s greatest achievements, yet it continues to advance at a rapid pace. Today’s anesthesia machines incorporate artificial intelligence monitoring systems, automated drug delivery mechanisms, and integrated patient data analytics. Understanding how these systems work and what safeguards protect patients is essential for healthcare professionals and patients alike. We’ll explore the technical specifications, regulatory oversight, and real-world performance data that determine whether anesthesia technology truly delivers on its safety promise.

How Modern Anesthesia Systems Work
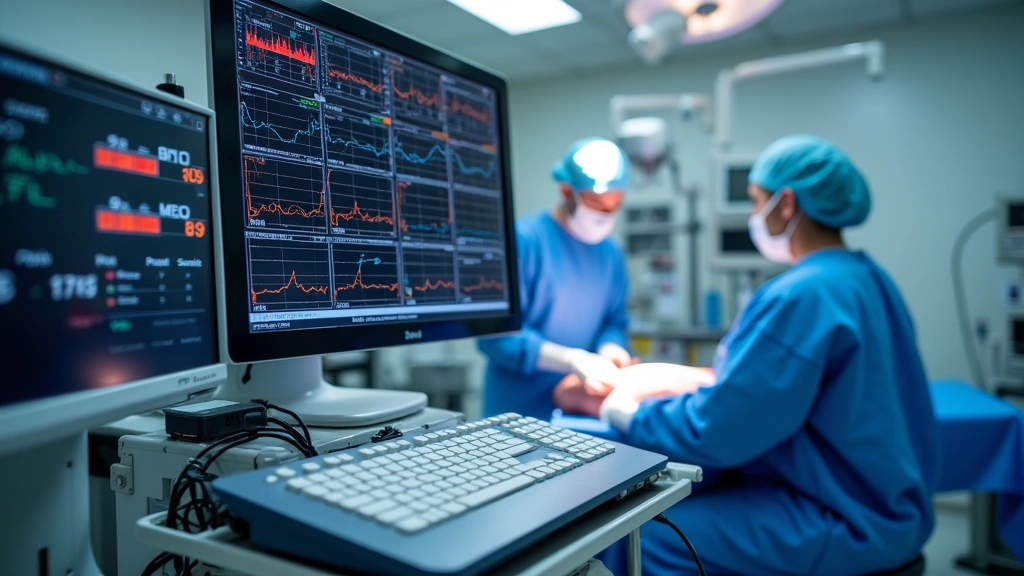
Contemporary anesthesia technology operates through a sophisticated integration of mechanical and electronic components designed to deliver precise drug concentrations while continuously monitoring patient vital signs. The core of any anesthesia system includes a vaporizer that converts liquid anesthetic agents into precise gaseous concentrations, a ventilator that controls respiratory parameters, and an elaborate sensor network that tracks oxygen saturation, carbon dioxide levels, heart rate, blood pressure, and neuromuscular function.
The anesthesia workstation—the central hub of the system—functions as an integrated platform combining gas delivery, patient monitoring, and electronic medical record integration. Modern systems like the Dräger Fabius and GE Aestiva incorporate touchscreen interfaces, electronic anesthetic agent measurement, and automated record-keeping. These machines can deliver volatile anesthetics (sevoflurane, desflurane, isoflurane) with precision to within 0.1% accuracy, far exceeding manual delivery capabilities.
When exploring artificial intelligence applications transforming modern medicine, anesthesia systems represent a prime example. Contemporary machines employ AI algorithms to predict patient responses, automatically adjust ventilation parameters based on lung compliance, and alert anesthesiologists to potential complications before they become critical. These predictive systems analyze hundreds of data points per second, identifying patterns that human operators might miss.
The delivery pathway follows strict protocols: compressed gases from tanks enter regulators that reduce pressure to working levels, flow through flowmeters calibrated with precision tolerances, pass through vaporizers that add volatile agents, and finally enter the patient circuit through breathing systems. Each component has redundant safety mechanisms—oxygen pressure failure devices automatically shut down other gases if oxygen pressure drops, preventing hypoxic mixtures from reaching the patient.
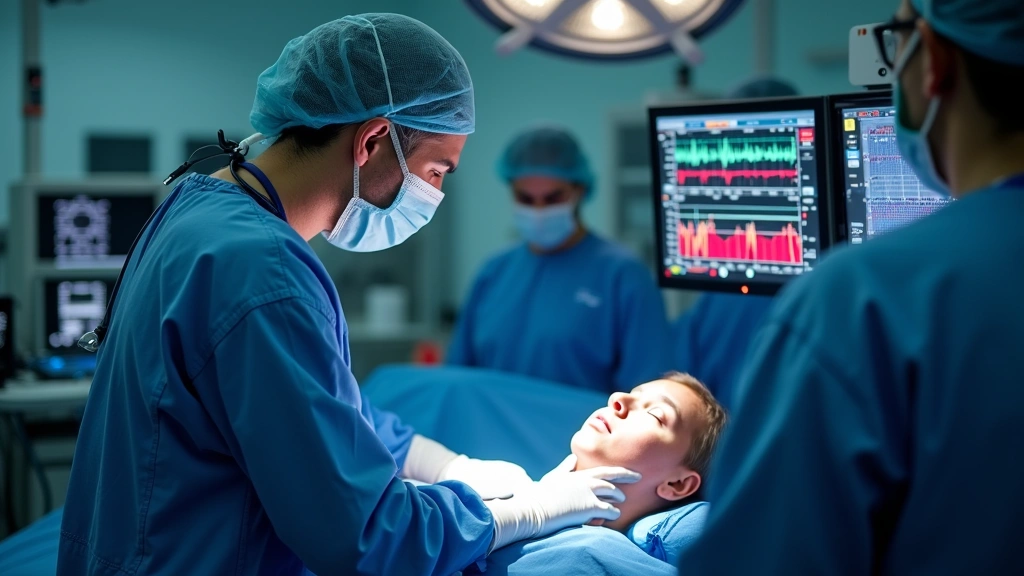
Regulatory Standards and Certifications
Anesthesia technology operates under stringent regulatory frameworks established by international bodies and national health authorities. The FDA (Food and Drug Administration) classifies anesthesia machines as Class II medical devices, requiring 510(k) premarket notification demonstrating substantial equivalence to predicate devices. This process mandates comprehensive testing of safety, performance, and design specifications before any system reaches clinical use.
The International Organization for Standardization (ISO) establishes the ISO 8835 series of standards specifically governing anesthesia equipment design, performance, and safety. These standards define everything from gas outlet configurations to alarm requirements, ensuring compatibility and safety across different manufacturers and models. ISO 5358 covers breathing system filters, while ISO 8835-1 specifically addresses anesthesia workstation design requirements.
The American Society of Anesthesiologists (ASA) publishes comprehensive standards for anesthesia equipment maintenance and use. ASA Standard 1 requires continuous monitoring of oxygenation, ventilation, circulation, and temperature during all general anesthetics. The organization mandates pre-use equipment checks documented on standardized checklists—typically the Anesthesia Equipment Checkout Recommendations created collaboratively with equipment manufacturers.
European regulations through the Medical Device Regulation (MDR) impose even stricter post-market surveillance requirements. Manufacturers must maintain comprehensive databases of adverse events, implement corrective action plans when issues emerge, and conduct regular risk assessments. These regulatory frameworks create multiple layers of oversight ensuring technology safety standards remain consistently high throughout anesthesia equipment lifecycles.
Clinical engineering departments at hospitals perform independent validation testing on all anesthesia systems, documenting performance against manufacturer specifications. This includes calibration verification of gas delivery accuracy, alarm system testing, and breathing circuit integrity checks. Many institutions exceed regulatory minimums, implementing additional safety protocols and maintenance schedules based on their risk assessments.
Safety Features and Fail-Safes
Modern anesthesia machines incorporate multiple redundant safety systems designed to prevent common accidents and failures. The oxygen pressure failure device represents the most critical fail-safe: if oxygen pressure drops below a threshold (typically 25 psi), the device automatically reduces or eliminates flow of other gases, preventing delivery of hypoxic mixtures that could cause patient harm. This mechanical safeguard requires no electricity or complex programming—it functions purely through pneumatic principles.
The second oxygen flush valve provides emergency high-flow oxygen delivery (up to 75 liters per minute) directly to the patient circuit, bypassing all other gas controls. This feature allows rapid oxygen delivery if other systems fail. The valve incorporates deliberate resistance to prevent accidental activation, requiring conscious engagement from the operator.
Volatile anesthetic agent delivery systems now employ electronic measurement and control rather than mechanical vaporizers alone. Anesthetic agent monitors measure actual delivered concentrations in real-time using infrared spectroscopy, immediately alerting operators if delivered concentrations deviate from set values. This technological advancement prevents overdose scenarios that could occur with mechanical vaporizers alone.
Alarm systems on modern anesthesia workstations operate with multiple redundancy layers. Auditory alarms vary in pitch and pattern according to alarm severity—critical alarms produce high-pitched, rapid sounds while advisory alarms use lower tones. Visual displays prominently highlight alarm conditions with color-coding (red for critical, yellow for warnings). These multi-modal alert systems ensure operators immediately recognize critical conditions regardless of ambient operating room noise.
Ventilator safety features include tidal volume monitoring with automatic adjustment, minute ventilation tracking, and airway pressure monitoring. If airway pressure exceeds safe limits (indicating obstruction or disconnection), alarms activate and ventilation parameters automatically adjust. Disconnect alarms detect separation between ventilator and patient circuit within seconds, preventing undetected apnea.
Gas supply integrity monitoring continuously verifies that supplied gases match selected values. If vaporizer settings don’t match delivered concentrations, or if wrong gases are connected, the system alerts operators. Oxygen concentration monitoring ensures delivered mixtures contain adequate oxygen—if oxygen concentration falls below safe minimums, immediate alarms activate regardless of operator attention.
Common Risks and Complications
Despite sophisticated safety systems, anesthesia technology still carries inherent risks that medical teams must actively manage. Hypoventilation represents one of the most common complications, where inadequate minute ventilation leads to carbon dioxide retention and respiratory acidosis. Modern ventilators include automatic minute ventilation monitoring, but operator error in setting parameters or failure to recognize alarms can still result in inadequate ventilation.
Hypoxemia—dangerously low blood oxygen levels—remains a primary concern in anesthesia. While oxygen monitoring systems provide real-time saturation data, equipment failures, circuit disconnections, or operator error can still result in hypoxic episodes. The critical safeguard involves pre-oxygenation protocols and continuous pulse oximetry monitoring, but human factors remain significant contributors to adverse outcomes.
Equipment malfunction, though rare with modern systems, can occur through manufacturing defects, maintenance failures, or operator error. Documented cases include vaporizer calibration drift (though rare with electronic systems), breathing circuit disconnections, and gas supply contamination. These incidents, when they occur, typically result from multiple system failures rather than single points of failure.
Drug administration errors represent a significant risk category where technology can help but doesn’t eliminate human error. Syringe swap incidents—where medications are inadvertently confused—have led to serious patient harm. Newer systems incorporate barcode scanning and electronic medication verification, but these technologies see variable adoption across institutions.
Anesthesia-related complications include malignant hyperthermia (a pharmacogenetic condition where certain anesthetic agents trigger life-threatening muscle metabolism), awareness under anesthesia (where patients regain consciousness during procedures), and anaphylactic reactions to anesthetic agents. While these complications relate more to pharmacology than technology, modern monitoring systems help detect these conditions earlier through vital sign changes and neuromuscular monitoring data.
Regulatory databases like the FDA’s MAUDE (Manufacturer and User Facility Device Experience) database document adverse events associated with anesthesia equipment. Analysis of this data shows that while serious injuries remain statistically rare given the millions of anesthetics administered annually, continued vigilance and technology improvements remain essential.
Expert Recommendations
Anesthesiologists and biomedical engineers who work with anesthesia technology consistently emphasize several key recommendations for maintaining safety. First, comprehensive pre-use equipment checks following ASA guidelines must occur before every anesthetic procedure. These standardized checklists verify gas supplies, breathing circuit integrity, alarm function, and monitoring system calibration. This ritualistic approach, though sometimes viewed as burdensome, has documented effectiveness in preventing equipment-related incidents.
Regular maintenance schedules established by manufacturers and regulatory bodies must be strictly followed. Annual calibration verification, preventive maintenance, and software updates ensure systems operate within design specifications. Many hospitals implement more frequent maintenance than regulatory minimums require, recognizing that prevention costs far less than managing adverse outcomes.
Staff training and competency verification represent critical safety components that technology cannot replace. Operators must understand how systems function, recognize alarm patterns, troubleshoot problems, and execute emergency procedures. Simulation-based training allows anesthesiologists and technicians to practice responses to equipment failures in safe environments before encountering real clinical situations.
Institutions should implement robust quality assurance programs including incident reporting, root cause analysis of adverse events, and implementation of corrective actions. These programs identify trends and systemic issues that might not be apparent from individual incidents. Learning from adverse events—both locally and through shared databases—continuously improves safety across the field.
Investment in newer technology systems incorporating advanced monitoring, automated safety features, and integrated electronic medical records provides measurable safety benefits. While cost represents a significant consideration, the safety improvements justify upgrades from older equipment. Organizations should balance technology advancement with staff training to ensure operators can effectively use new capabilities.
Interdisciplinary collaboration between anesthesiologists, biomedical engineers, and hospital administrators ensures that safety considerations inform equipment procurement decisions. Technical specifications matter, but real-world usability and integration with existing systems also significantly impact safety outcomes. When considering how technology enhances safety in complex systems, anesthesia equipment demonstrates these principles clearly.
Technology Advancements Improving Safety
Recent technological innovations continue advancing anesthesia safety beyond previous capabilities. Closed-loop anesthesia systems represent a frontier development where computers automatically adjust anesthetic agent delivery based on real-time patient response monitoring. These systems measure processed EEG signals indicating depth of anesthesia and automatically adjust propofol or volatile agent delivery to maintain target levels, reducing under- and over-dosing risks.
Artificial intelligence systems analyzing anesthesia data can predict patient deterioration minutes before clinical signs become obvious. Machine learning algorithms trained on thousands of anesthetics identify subtle pattern changes in vital signs, gas exchange, and cardiac function that precede critical events. These predictive capabilities allow proactive intervention before emergencies develop.
Enhanced monitoring technologies including non-invasive cardiac output monitoring, cerebral oxygenation monitoring, and advanced neuromuscular monitoring provide unprecedented insight into patient physiology during anesthesia. These technologies help anesthesiologists detect complications earlier and titrate therapy more precisely.
Integration of anesthesia workstations with electronic medical records and pharmacy systems enables automated medication verification and documentation. Barcode scanning and electronic verification reduce medication errors, while automatic documentation reduces transcription errors and improves data quality for quality improvement initiatives.
Portable anesthesia delivery systems incorporating modern safety features extend safe anesthesia practice beyond traditional operating rooms. These systems, used for procedures in remote locations or austere environments, incorporate essential safety features while remaining transportable. This democratization of safe anesthesia technology improves access to surgical care in resource-limited settings.
Simulation and virtual reality training platforms allow anesthesiologists to practice emergency scenarios and equipment troubleshooting without patient risk. These educational tools, informed by how professionals learn technical skills efficiently, accelerate competency development and improve safety outcomes.
Remote monitoring and telemedicine integration enables experienced anesthesiologists to advise on complex cases from distant locations. While not replacing on-site presence, these capabilities provide consultation support and quality oversight that improves decision-making in challenging situations.
Blockchain-based verification systems for anesthetic agent authenticity prevent counterfeit medication incidents. As global pharmaceutical supply chains grow increasingly complex, cryptographic verification ensures that delivered medications are authentic and have maintained proper storage conditions.
FAQ
What makes anesthesia technology safer than it was decades ago?
Modern anesthesia systems incorporate electronic monitoring, automated safety features, redundant fail-safes, and real-time data analysis that weren’t possible with mechanical equipment. Electronic anesthetic agent measurement eliminates vaporizer calibration drift. Continuous physiologic monitoring detects problems within seconds rather than minutes. Integrated alarm systems with multiple sensory modalities ensure operators immediately recognize critical conditions. These advancements have reduced anesthesia-related mortality from historical rates of 1 per 10,000 to current rates below 1 per 100,000 in developed healthcare systems.
Can anesthesia equipment fail unexpectedly?
While catastrophic failures are extremely rare with modern equipment, component failures can occur. Mechanical components can wear, electronic systems can malfunction, and software can contain bugs. However, modern systems incorporate multiple redundant safety mechanisms so that single component failures don’t result in dangerous situations. This “defense in depth” approach means that typically multiple failures must occur simultaneously to create unsafe conditions. Rigorous maintenance schedules, pre-use checks, and regulatory oversight minimize failure risks.
How do anesthesia machines prevent giving patients the wrong gas mixture?
Multiple safety systems prevent hypoxic mixtures. Oxygen pressure failure devices automatically cut off other gases if oxygen pressure drops. Electronic oxygen concentration monitoring continuously verifies delivered oxygen levels and alarms if concentrations fall below safe minimums. Flowmeters display oxygen flow prominently. Modern systems measure actual delivered concentrations using infrared spectroscopy and immediately alert operators to deviations. These redundant systems mean that hypoxic gas delivery requires multiple simultaneous system failures.
What should patients ask their anesthesiologist about equipment safety?
Patients can ask whether the facility performs pre-use equipment checks, how frequently equipment undergoes maintenance, and what monitoring will be used during their procedure. Questions about the anesthesiologist’s experience with the specific equipment and facility protocols for equipment problems are appropriate. Most facilities maintain excellent safety records, and anesthesiologists welcome questions demonstrating patient engagement in their care.
Are older anesthesia machines less safe than newer models?
While newer systems incorporate advanced features like closed-loop delivery and AI monitoring, well-maintained older equipment with proper operator training remains safe. The fundamental safety principles—oxygen fail-safe devices, continuous monitoring, and redundant alarms—have been incorporated in quality anesthesia machines for decades. However, newer systems do offer enhanced safety through automated features that reduce operator workload and improve precision. When considering how to evaluate technology upgrades, the same principles apply to medical equipment: newer isn’t always necessary, but targeted upgrades addressing specific safety concerns provide clear benefits.
How are anesthesia machines tested for safety?
Manufacturers conduct extensive testing including bench testing of component performance, animal studies documenting physiologic effects, and clinical trials in human subjects before regulatory approval. Post-market surveillance through adverse event databases continues monitoring safety. Clinical engineering departments at hospitals perform independent testing verifying performance against specifications. Regulatory bodies conduct inspections and audit manufacturer quality systems. This multi-layered testing and oversight ensures comprehensive safety evaluation.
What role does artificial intelligence play in anesthesia safety?
AI systems analyze real-time patient data to predict deterioration, optimize anesthetic dosing, and detect equipment problems. Machine learning algorithms identify subtle physiologic patterns that precede critical events, allowing proactive intervention. Closed-loop systems automatically adjust anesthetic delivery based on patient response, reducing human error. However, AI augments rather than replaces human judgment—anesthesiologists remain responsible for clinical decisions and oversight.