Top Anesthesia Tech Gadgets: Expert Opinions on Equipment That Matters
The anesthesia technology landscape has undergone a dramatic transformation over the past decade. Modern anesthesia tech encompasses sophisticated monitoring systems, precision delivery devices, and AI-driven safety platforms that fundamentally change how anesthesiologists approach patient care. Whether you’re exploring anesthesia tech jobs or seeking to understand the equipment professionals rely on daily, this comprehensive guide breaks down the gadgets reshaping operating rooms worldwide.
Professional anesthesia technologists and certified registered nurse anesthetists (CRNAs) now operate within an ecosystem of interconnected devices that demand both technical proficiency and continuous learning. The intersection of healthcare and technology creates unique career opportunities for those passionate about both fields. Understanding the tools of the trade isn’t just academic—it directly impacts patient outcomes and professional competency in anesthesia technology positions.
Advanced Anesthesia Delivery Systems
Modern anesthesia delivery systems represent the pinnacle of precision engineering in healthcare technology. The latest platforms combine volumetric and flow-controlled ventilation with integrated anesthetic agent delivery, creating seamless workflows that minimize human error and optimize drug administration.
Closed-Loop Anesthesia Systems have emerged as game-changers in operating room efficiency. These systems utilize real-time feedback mechanisms to automatically adjust anesthetic agent concentrations based on processed electroencephalogram (EEG) data and hemodynamic parameters. Industry leaders like Dräger and Philips Healthcare have pioneered systems that reduce anesthetic consumption by 15-30% while maintaining optimal depth of anesthesia.
The Aisys CS2 system from GE Healthcare exemplifies this technology, featuring:
- Integrated processed EEG monitoring with automated anesthetic titration
- Dual-agent capability allowing simultaneous volatile anesthetic delivery
- Real-time gas monitoring with predictive analytics
- Touch-screen interface with customizable workflows
- Seamless electronic health record (EHR) integration
These systems demand specialized training, making knowledge of advanced anesthesia delivery crucial for anyone pursuing anesthesia tech career opportunities. Technologists must understand ventilation modes, gas mixing principles, and troubleshooting protocols to support anesthesia providers effectively.

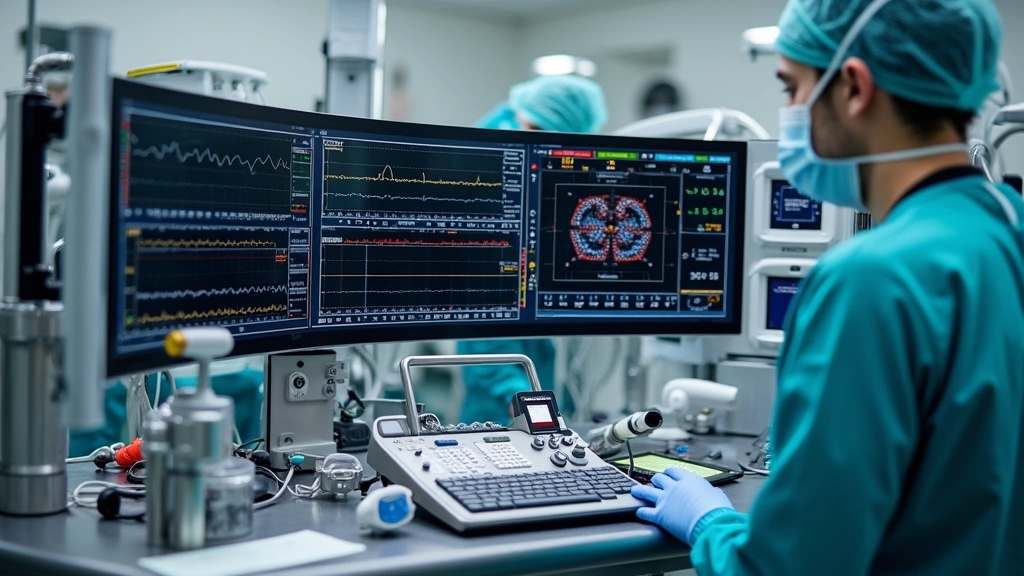
Patient Monitoring Platforms
Comprehensive patient monitoring forms the backbone of safe anesthesia practice. Contemporary monitoring platforms integrate multiple physiological parameters into unified displays, enabling anesthesia teams to detect subtle changes before they become critical issues.
Multiparameter Patient Monitors now incorporate:
- Electrocardiography (ECG) with arrhythmia detection algorithms
- Non-invasive blood pressure monitoring with oscillometric and auscultatory methods
- Pulse oximetry with motion artifact rejection
- Capnography with end-tidal carbon dioxide trending
- Temperature monitoring with predictive hypothermia alerts
- Neuromuscular transmission monitoring via acceleromyography
The GE CARESCAPE Monitor B850 represents state-of-the-art integration, combining traditional vital sign monitoring with advanced hemodynamic parameters including stroke volume variation and pulse pressure variation—metrics that guide fluid management decisions during major surgery.
Anesthesia technologists specializing in monitoring systems must understand signal acquisition, artifact recognition, and alarm management. This expertise directly supports anesthesia tech positions in academic medical centers and large surgical facilities where monitoring complexity reaches its highest levels.
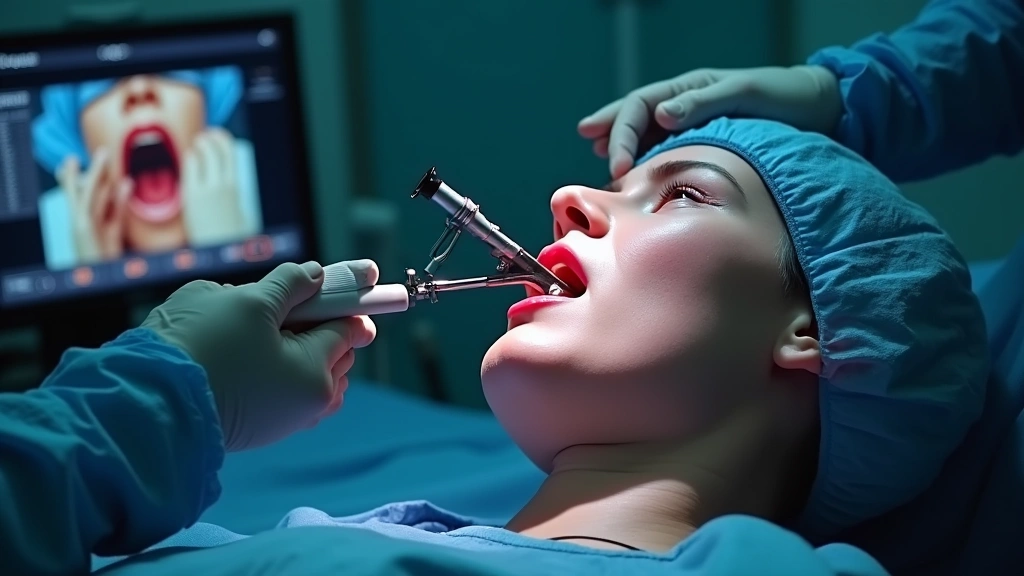
Airway Management Technology
Securing and maintaining a patent airway remains anesthesia’s most critical responsibility. Modern airway management devices have evolved from basic laryngoscopes to sophisticated visualization and intubation systems that improve first-pass success rates and reduce airway complications.
Video Laryngoscopes have revolutionized intubation technique. Devices like the McGrath MAC and Storz C-MAC provide high-definition visualization of vocal cord anatomy, enabling intubation in previously difficult airway scenarios. Key advantages include:
- Superior visualization angle (up to 60 degrees)
- Real-time video recording for quality assurance and training
- Reduced post-operative sore throat incidence
- Faster intubation times compared to traditional direct laryngoscopy
- Enhanced safety in patients with anticipated difficult airways
Supraglottic airway devices (SADs) like the LMA Supreme and i-gel represent alternatives to endotracheal intubation, offering faster placement times and reduced airway trauma. Understanding the indications, techniques, and complications associated with each device is essential for anesthesia tech professionals managing difficult airway situations.
Fiber-optic bronchoscopes remain invaluable for awake fiberoptic intubation in high-risk patients. These precision instruments demand meticulous care, sterilization protocols, and technical knowledge to maintain functionality and prevent cross-contamination.
Data Integration and Safety Systems
Modern operating rooms increasingly feature integrated data management systems that consolidate information from anesthesia delivery systems, monitors, electronic health records, and peripheral devices into unified platforms. These OR Integration Systems enhance patient safety through comprehensive documentation and real-time decision support.
Anesthesia Information Management Systems (AIMS) automatically capture vital signs, medication administration, and clinical events, creating detailed intraoperative records without manual transcription. Benefits include:
- Reduced documentation burden on anesthesia providers
- Enhanced medication error detection through barcode verification
- Real-time alerts for critical value thresholds
- Automated compliance with Joint Commission safety standards
- Improved data quality for quality improvement initiatives
Artificial intelligence integration within these systems now enables predictive analytics identifying patients at risk for intraoperative hypotension, excessive bleeding, or other complications. The Verge’s healthcare technology coverage frequently highlights how machine learning algorithms are transforming clinical decision-making in perioperative settings.
For technologists interested in the intersection of anesthesia and advanced technology, exploring software development pathways can open doors to careers designing and implementing these complex systems. The demand for professionals who understand both clinical workflows and programming continues accelerating.
Portable and Point-of-Care Devices
Beyond the operating room, portable anesthesia technology serves critical roles in emergency departments, intensive care units, and remote surgical settings. These devices prioritize durability, battery efficiency, and rapid deployment.
Portable Anesthesia Workstations enable anesthesia delivery in non-traditional settings. The Penlon Portable Anesthesia Workstation, for example, operates without electricity, utilizing pneumatic power sources ideal for field hospitals and developing nations. Features include:
- Self-contained oxygen and anesthetic agent delivery
- Minimal maintenance requirements
- Lightweight construction (under 30 kg)
- Compatibility with standard monitoring equipment
- Cost-effectiveness for resource-limited settings
Point-of-Care Testing Devices provide immediate laboratory results during anesthesia. Blood gas analyzers, coagulation monitors, and glucose meters enable real-time decision-making without laboratory turnaround delays. The iSTAT portable clinical analyzer delivers comprehensive metabolic panels within 90 seconds, critical for managing hemodynamic stability during major surgery.
Anesthesia technologists supporting these portable systems must understand maintenance protocols, battery management, and troubleshooting in challenging environments—skills increasingly valuable as healthcare expands into telemedicine and remote surgical capabilities.
Training and Simulation Equipment
Simulation technology has become integral to anesthesia education and competency maintenance. High-fidelity patient simulators combined with virtual reality platforms create immersive learning environments where trainees develop skills safely before encountering real patients.
Full-Body Patient Simulators like the SimMan 3G and CAE Lucina respond realistically to anesthetic interventions, displaying physiological changes that mirror actual patient responses. These systems feature:
- Programmable cardiovascular responses to medications
- Realistic airway anatomy for intubation practice
- Lung compliance changes reflecting ventilation strategies
- Synchronized monitoring displays matching operating room equipment
- Wireless connectivity for remote instructor control
Virtual reality anesthesia simulations offer advantages in accessibility and cost-effectiveness. Platforms enabling practice of difficult airway management, regional anesthesia techniques, and crisis scenarios allow learners to repeat procedures unlimited times without equipment constraints.
For those pursuing education in anesthesia technology, understanding simulation capabilities directly informs curriculum development and competency assessment. Selecting appropriate computing devices for educational pursuits becomes relevant when engaging with virtual simulation platforms requiring substantial processing power.
Procedural Training Stations focusing on regional anesthesia techniques utilize ultrasound simulators and anatomical models to teach nerve blocks, epidural placement, and spinal injection techniques. These hands-on stations build manual dexterity and anatomical understanding essential for clinical competence.
The integration of simulation into anesthesia tech job requirements continues expanding, with many employers now mandating simulation-based competency verification before independent practice.
Understanding emerging technology like augmented reality (AR) guidance systems for regional anesthesia represents the frontier of anesthesia education. These systems overlay ultrasound anatomy with needle trajectory predictions, improving accuracy and reducing complications.
FAQ
What qualifications do anesthesia technologists need to operate advanced equipment?
Certification through the American Society of Anesthesiologists (ASA) requires completion of an accredited anesthesia technician program (typically 12-24 months), followed by passing the Certified Anesthesia Technician (CAT) examination. Many advanced gadgets require manufacturer-specific training beyond baseline certification. Continuing education credits maintain licensure and ensure competency with evolving technology.
How often is anesthesia equipment updated in modern hospitals?
Major anesthesia delivery systems typically remain in service 8-12 years before replacement. However, software updates, monitoring module upgrades, and peripheral device additions occur continuously. Hospitals often implement new technologies in phases, requiring technologists to maintain proficiency across multiple equipment generations simultaneously.
Which anesthesia tech skills are most in-demand currently?
Expertise in closed-loop anesthesia systems, AIMS operation, difficult airway management equipment, and OR integration platforms commands premium compensation. Additionally, knowledge of point-of-care testing devices and remote monitoring capabilities increasingly separates competitive candidates in the job market.
Can anesthesia technologists transition into software or biomedical engineering roles?
Absolutely. Clinical experience combined with programming language expertise positions technologists uniquely for biomedical engineering careers. Many medical device companies specifically recruit from clinical backgrounds, valuing the workflow insights that inform better product design.
What safety standards govern anesthesia technology?
The FDA regulates anesthesia delivery systems and monitors as medical devices, requiring compliance with ISO standards for electrical safety, accuracy, and reliability. Additionally, the Joint Commission establishes accreditation standards for anesthesia services, and the American Society of Anesthesiologists publishes equipment maintenance and monitoring guidelines that healthcare facilities must follow.
How does artificial intelligence impact anesthesia technologist roles?
AI integration in predictive analytics and automated drug delivery enhances technologist responsibilities rather than replacing them. Professionals must now understand algorithm outputs, validate system recommendations, and intervene when AI-driven decisions require clinical judgment. This evolution expands the intellectual demands of the profession while increasing career advancement opportunities.